How a Wound Care Specialist Can Help Manage Diabetic Foot Ulcers
Whether you’ve noticed a new sore or are dealing with a stubborn, chronic wound, don’t delay — professional care gives you the best chance at recovery and a healthier future.
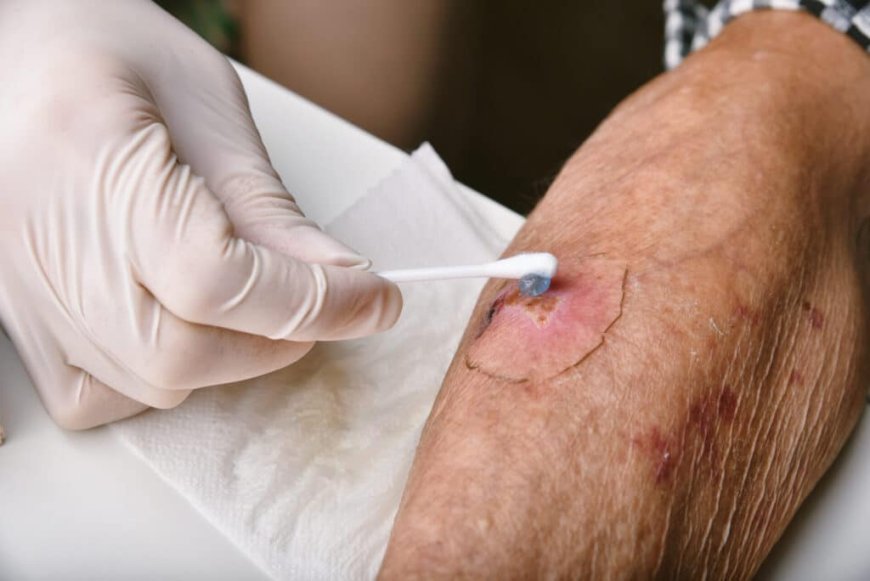
Diabetic foot ulcers are one of the most serious complications associated with uncontrolled or poorly managed diabetes. These open sores can be slow to heal and prone to infection, often leading to hospitalization and, in severe cases, amputation. The good news is that early and consistent care from a qualified wound care specialist can dramatically improve healing outcomes and prevent life-altering consequences.
What Are Diabetic Foot Ulcers?
A diabetic foot ulcer is an open wound or sore that occurs on the feet, typically on the sole, toes, or heel. They develop due to a combination of poor circulation, nerve damage (neuropathy), and immune system issues common in people with diabetes. Because of reduced sensation, many individuals dont notice the sore until it worsens.
Key characteristics of diabetic foot ulcers:
-
May start as a blister or small cut
-
Often painless due to nerve damage
-
Can appear red, swollen, or weeping fluid
-
Prone to bacterial infection
-
Frequently occur under pressure points like the ball of the foot
Why Diabetic Foot Ulcers Are Dangerous
Without prompt treatment, diabetic foot ulcers can escalate into severe infections, cellulitis, gangrene, or bone infections (osteomyelitis). These complications may lead to prolonged hospital stays, multiple surgeries, or amputation.
Major risks include:
-
Delayed wound healing
-
Deep tissue or bone infections
-
Poor circulation hindering recovery
-
Loss of mobility or limb function
Seeing a wound care specialist early can reduce these risks and speed up the healing process.
How a Wound Care Specialist Diagnoses Diabetic Foot Ulcers
At your first visit, a wound care specialist performs a comprehensive evaluation to determine the severity of your ulcer and identify any complications.
Theyll assess:
-
Wound size, depth, and location
-
Presence of infection or dead tissue
-
Signs of circulation issues
-
Sensory function in the foot
-
Blood sugar levels and medical history
Diagnostic tests like X-rays or wound cultures may be ordered if infection or bone involvement is suspected.
Treatment Techniques Used by Wound Care Specialists
Modern diabetic wound care focuses on improving blood flow, removing dead tissue, preventing infection, and stimulating new tissue growth. A wound care specialist creates a personalized plan based on your ulcers stage and your overall health.
Standard treatments include:
-
Debridement to clean away dead tissue
-
Advanced wound dressings to maintain a moist, healing environment
-
Antibiotic therapy for infections
-
Blood sugar management coordination with your primary care provider
-
Offloading techniques to reduce pressure on the wound (special footwear, orthotics, or casts)
Advanced Therapies for Hard-to-Heal Diabetic Ulcers
When diabetic foot ulcers resist standard care, a wound care specialist may recommend advanced therapies to support faster, complication-free healing.
Options include:
-
Negative Pressure Wound Therapy (NPWT): Uses suction to remove drainage and boost blood flow
-
Hyperbaric Oxygen Therapy: Delivers oxygen under pressure to accelerate tissue repair
-
Bioengineered Skin Substitutes: Artificial skin grafts to cover the wound and promote healing
-
Growth Factor Therapy: Topical treatments to stimulate cell regeneration
Why Blood Sugar Control Matters
A crucial part of healing diabetic wounds is controlling blood glucose levels. High blood sugar damages blood vessels, impairs immune response, and slows tissue repair.
A wound care specialist will:
-
Collaborate with your diabetes care team
-
Recommend dietary adjustments
-
Suggest activity modifications
-
Monitor healing in relation to glucose trends
Without blood sugar control, even the most advanced wound therapies will have limited success.
Prevention Strategies Recommended by Wound Care Specialists
Preventing diabetic foot ulcers is always better than treating them. A wound care specialist offers valuable advice to help you avoid future wounds.
Prevention tips include:
-
Daily foot checks for blisters, cuts, or color changes
-
Wearing protective, properly fitted footwear
-
Avoiding walking barefoot
-
Maintaining good blood sugar control
-
Regular foot exams by a healthcare professional
-
Moisturizing feet but avoiding lotion between toes
-
Stopping smoking to improve circulation
Signs You Should See a Wound Care Specialist for a Diabetic Foot Ulcer
Early intervention makes a dramatic difference in diabetic wound outcomes. See a specialist immediately if you notice:
-
A sore or ulcer on your foot lasting more than 7 days
-
Signs of infection like redness, swelling, or foul odor
-
Increasing pain or drainage from the wound
-
Black, dead, or discolored tissue
-
Fever, chills, or general illness symptoms
Prompt professional care can prevent serious, sometimes irreversible complications.
Benefits of Working With a Wound Care Specialist
Partnering with a wound care specialist gives you access to specialized tools and techniques you wont find in a general clinic or emergency room.
Benefits include:
-
Faster wound closure rates
-
Lower risk of serious infections
-
Customized offloading strategies
-
Coordinated care with diabetes specialists
-
Access to advanced treatments like NPWT or hyperbaric oxygen therapy
-
Education on foot care and wound prevention
FAQs About Diabetic Foot Ulcers and Wound Care Specialists
Q1: How long does it take for a diabetic foot ulcer to heal?
Healing time varies based on the ulcers size, depth, infection status, and blood sugar control. With expert care, many ulcers improve within 46 weeks, while complex wounds may take several months.
Q2: Can diabetic foot ulcers heal without specialist care?
Some mild ulcers may improve with basic care, but most require professional management to prevent infections and complications. Delaying treatment increases the risk of serious outcomes.
Q3: Will I need surgery for a diabetic ulcer?
Surgery is considered when wounds dont respond to conservative care, especially if theres bone involvement or severe tissue loss. A wound care specialist will exhaust non-surgical options first.
Q4: What can I do at home to support healing?
Keep your blood sugar well-managed, follow your dressing change instructions, avoid putting pressure on the wound, and check your feet daily for new sores or signs of infection.
Q5: Are diabetic foot ulcers covered by insurance?
Most insurance plans cover specialist wound care services, especially for chronic wounds. Confirm coverage details with your provider ahead of your visit.
Final Thoughts
Diabetic foot ulcers are a serious health risk, but with early and expert care from a wound care specialist, you can heal faster, avoid hospitalization, and dramatically reduce your risk of amputation.































